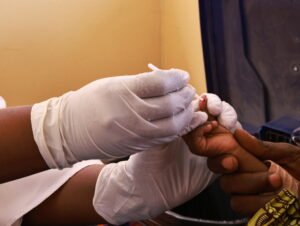
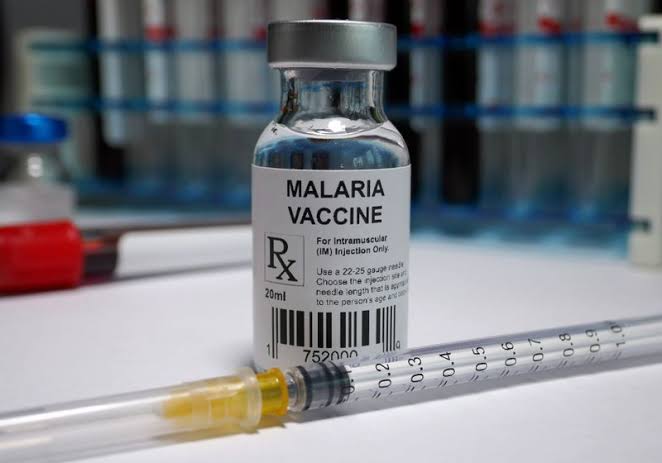
WHO approves first malaria vaccine for children
Modupe Shodeinde
The World Health Organisation (WHO) is recommending widespread use of the world’s first malaria vaccine for the decades-long battle against the deadly disease for children at risk.
The vaccine is geared towards children, in sub-Saharan Africa and other regions with moderate to high transmission.
The recommendation to begin using the RTS, S vaccine, is based an ongoing pilot programme set up by WHO and partners in Ghana, Kenya and Malawi, that has reached more than 800,000 children since 2019.
“The long-awaited malaria vaccine for children is a breakthrough for science, child health and malaria control,” WHO Director-General, Tedros Ghebreyesus, said at a news conference at WHO Headquarters in Geneva.
“Using this vaccine on top of existing tools to prevent malaria could save tens of thousands of young lives each year,” he said.
Ghebreyesus said the world had made “incredible progress” in the fight against malaria in the past two decades.
The malaria parasite is mostly transmitted by infective mosquitoes and carried in the blood, after being bitten.
It is not contagious person-to-person, and symptoms include a fever of flu-like illness, nausea and vomiting, and if left untreated, it can be fatal, killing more than 400,000 each year worldwide.
Malaria remains a primary cause of childhood illness and death in sub-Saharan Africa. More than 260,000 African children under the age of five die from malaria annually.
Also speaking at the news conference, WHO Regional Director for Africa, Dr Matshidiso Moeti, said that “for centuries, malaria has stalked sub-Saharan Africa, causing immense personal suffering.”
“We have long hoped for an effective malaria vaccine and now for the first time ever, we have such a vaccine recommended for widespread use.”
Moeti said today’s recommendation “offers a glimmer of hope for the continent which shoulders the heaviest burden of the disease and we expect many more African children to be protected from malaria and grow into healthy adults.”
WHO Director-General further said, “This is a powerful new tool, but like COVID-19 vaccines, it’s not the only tool.
“Vaccination against malaria does not replace or reduce the need for other measures, including bednets, or seeking care for fever,”